Have you ever felt a sharp throb in your tooth that won’t quit? It’s unsettling when dental issues arise. Many people face this, often wondering about the hidden processes behind the pain. This post dives into the journey from a simple tooth infection to a full abscess. We’ll break it down step by step, sharing insights to help you stay ahead of problems.
What Is a Tooth Infection?
Tooth infections start small but can escalate fast. Bacteria play the main role here. They enter through cracks or decay. Poor oral hygiene lets them thrive. Food particles and plaque build up. Over time, this erodes enamel. The infection reaches deeper layers. Nerves and blood vessels get involved. This is where trouble brews.
Dental caries, or cavities, often kick things off. Trauma from injury can also open the door. Once inside, bacteria multiply. The body’s immune response fights back. But if unchecked, it spreads. Pulp, the tooth’s core, becomes inflamed. This stage is pulpitis. Pain signals the issue. Ignoring it worsens matters.
The Stages of Abscess Formation
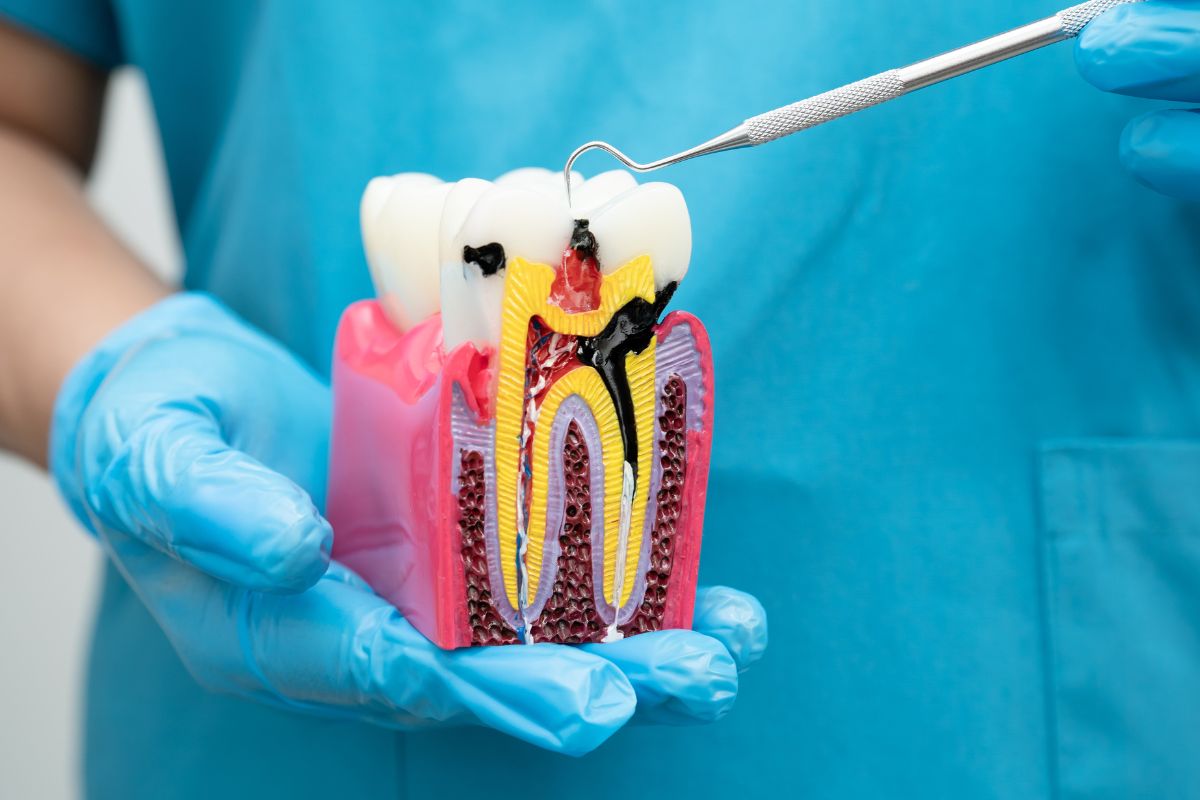
Abscesses don’t appear overnight. They follow a progression. First, enamel decays. Bacteria attack the hard outer layer. Next, they hit dentin. This softer part amplifies sensitivity. Then, pulp infection sets in. Bacteria invade the center. Pus forms as white blood cells battle.
The infection pushes to the root tip. It exits through the apex. Surrounding bone and tissue react. A pocket of pus develops. This is the periapical abscess. Gums may swell. In some cases, it spreads to nearby areas. Periodontal abscesses form between tooth and gum. Both types stem from untreated infections.
Bacteria like Streptococcus mutans drive this. They produce acids that break down tissues. The abscess acts as a containment. But pressure builds. Without relief, it can burst or spread further. Early detection stops this chain.
Common Symptoms and Warning Signs
Spotting symptoms early makes a difference. Throbbing pain is a key sign. It worsens with biting or heat. Swelling around the face or jaw appears. Gums turn red and tender. Fever or chills may occur. Bad breath lingers despite brushing.
Lymph nodes swell under the jaw. A pimple-like bump on gums signals pus. Bitter taste from drainage happens. Headaches or ear pain can mimic other issues. These signs vary by person. But they all point to infection. Don’t dismiss them as minor aches.
If pain disrupts sleep, act fast. Delaying invites complications. Infections can affect overall health. Heart or brain risks rise in rare cases. Listen to your body. Simple checks at home help, like gentle tapping on teeth.
For those dealing with persistent tooth pain, treatments like root canal therapy in Austin, MN can address the root cause effectively. It removes infected pulp and seals the tooth. This preserves your natural smile.
Prevention Strategies for Healthy Teeth
Prevention beats cure every time. Brush twice daily with fluoride toothpaste. Floss to remove hidden debris. Limit sugary snacks. Regular check-ups catch issues early. Use mouthwash for extra protection.
Healthy habits reduce risks. Stay hydrated to wash away bacteria. Chew sugar-free gum to boost saliva. Avoid tobacco; it weakens gums. Protective gear during sports prevents trauma. Balanced diet supports enamel strength.
Home remedies offer temporary relief. Saltwater rinses soothe inflammation. Cold packs ease swelling. But they’re not substitutes for care. Persistent problems need expert input.
Trending FAQs on Dental Abscess Formation
People often search for quick answers on this topic. Here are some trending FAQs based on common Google queries, with clear explanations:
- What causes a dental abscess to form? It starts with bacteria entering the tooth through decay or cracks, infecting the pulp and leading to pus buildup at the root.
- What are the stages of a tooth abscess? It begins with enamel decay, moves to dentin and pulp infection, then forms a pus pocket at the root tip.
- How do you know if you have a tooth abscess? Look for severe pain, swelling, fever, or a gum pimple; these indicate infection needing attention.
- Can a tooth abscess go away on its own? Rarely; most require treatment to drain pus and remove infection, as it can worsen without intervention.
- What happens if a tooth abscess is left untreated? It may spread to jaw, neck, or bloodstream, causing serious health issues like sepsis.
These questions highlight widespread concerns. Addressing them builds trust.
Key Statistics on Dental Infections
Dental issues affect many Americans. Here’s a table with relevant stats:
| Statistic | Detail | Source |
|---|---|---|
| Annual ER Visits for Abscesses | About 200,000 people seek emergency care yearly. | Impressions Dental |
| Untreated Caries in Adults (20-44) | 26% have untreated tooth decay. | CDC |
| Untreated Caries in Children (5-19) | 13% face untreated dental caries. | CDC |
| Hospital Admissions for Infections | 1 in 2,600 people hospitalized annually. | NCBI |
| Adults Seeking Care for Infections | 13% seek help within 4 years. | NCBI |
These numbers show the prevalence. Early action reduces these risks.
Infections demand prompt care. Delaying can lead to tooth loss. Endodontic options save teeth. They clean out bacteria effectively.
When facing these issues, consulting a dentist in Austin, MN makes sense. They offer tailored advice in a welcoming setting. It’s about feeling comfortable while getting expert help.
Options like endodontics target the problem. They restore function without extraction. This keeps your bite strong.
Wrapping Up: Take Charge of Your Oral Health
Dental health ties into overall well-being. Understanding abscess formation empowers you. From infection start to prevention, knowledge guides better choices. Stay vigilant with symptoms. Adopt daily habits for lasting protection. If concerns arise, don’t hesitate to schedule an appointment. Your smile deserves it.